|
||
|
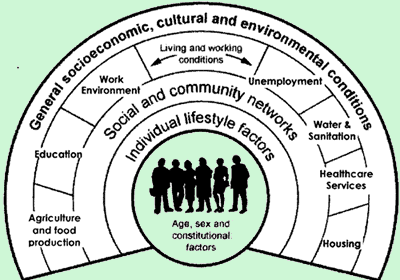
We live longer, our children grow taller than us and the scourge of diseases such as rubella, diphtheria, whooping cough and polio have yielded to mass vaccination. Diseases of poor living conditions such as typhoid, tuberculosis and pneumonia are forgotten, and the ricket-raddled urchin from poor nutrition is long banished to the pages of a Dickensian novel. But wait a minute, although life expectancy has risen over the last century, not all life is lived in good health. Our healthy life expectancy - the length of life free from ill health and disability - has not been rising at the same rate because the added years of life have been filled for some with chronic illness or disability. The proportion of people reporting a long-standing illness has grown steadily, rising from 15 per cent to 22 per cent since 1975. So what is going on? Much of it is to do with health inequalities. An unskilled worker is more than twice as likely to die from strokes, heart disease, lung cancer, accidents and violence, or suicide than is the professional worker. See for yourself that schoolchildren on regeneration estates are physically smaller, and suffer more from asthma than those in leafy suburbs. Health inequalities have been recognised since the social and public health reform of the nineteenth century, when Chadwick and Rowntree began to document them. It was evidence on social inequalities and of inadequate access to health care in Britain that provided the pressure to set up the welfare state and the National Health Service in the post-war period. The landmark Beveridge Report in 1942 set out a national programme of policies and services to combat the "five giants of Want, Disease, Ignorance, Squalor and Idleness Unfortunately, we seem to need to keep revisiting these causes of ill health. An assessment in the mid-1970s showed that Britain was slipping behind other countries in health improvement, despite 30 years of the welfare state. Fearing that persistent health inequalities were to blame, led to the Black Report in 1980 on Inequalities in Health. More recently, in 1998, we have had the Acheson Report on Inequalities in Health, a devastating report that firmly identified social exclusion as a major factor in the ill health of a significant proportion of our population, and correlated poor health with poor housing, poor diet and low incomes.
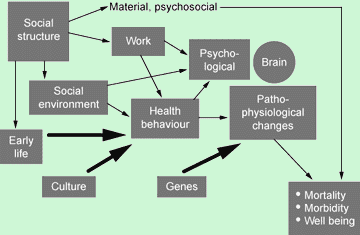
Unemployment is a major factor leading to ill health. Loss of income could result in a drop in living conditions such as poor diet, inadequate clothing and heating, and poor housing, leading to an increased incidence of bronchitis, cardiovascular disorders and low birth weight coupled with poor infant growth. But there are also the psychological and social losses like loss of identity, status and self esteem; reduction in decision-making/control and in social contacts; loss of timestructure, security and sense of future; and an increase in threatening/humiliating experiences. Psycho-social stress is on the increase leading to physiological changes such as high blood pressure, and altered mental states such as anxiety, depression and apathy. The quality of the social environment is worst where financial deprivation is greatest, such as the inner cities. Recent research suggests that, in addition to the ill effects due to absolute poverty, societies in which there is a wide gap between the rich and the poor suffer additional social problems through high rates of violence and crime, and truancy. People with good social networks live longer, are at reduced risk of coronary heart disease, are less likely to report being depressed, or to suffer a recurrence of cancer and are less susceptible to infectious illness than those with poor networks.
Mark Fisher - Permaculture Design course handout notes www.self-willed-land.org.uk mark.fisher@self-willed-land.org.uk |